
Structures and systems influence how power and resources are distributed within communities through policies, practices, and cultural norms. These resources are often not distributed equitably due to root causes such as racism, sexism, classism, and heterosexism.
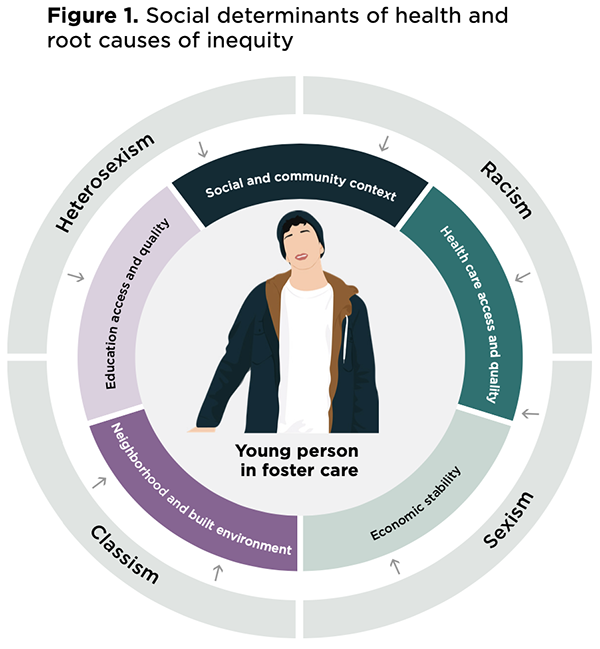 Research finds that sexual and reproductive health outcomes among young people in foster care are worse than among the general population (for example, young people in foster care report first having sex at younger ages than the general population, and young women in foster care experience higher rates of teen pregnancy).[6] However, research also shows that understanding and addressing the ways in which social determinants of health influence the sexual and reproductive health of young people in foster care is imperative to providing them with effective services and improving outcomes related to their sexual and reproductive health. Youth in foster care experience unique conditions that caseworkers and others working within the foster care system should be aware of and mindful toward, such as separation from family of origin, decreased social support,[7] placement instability, and lack of voice and bodily autonomy over medical decisions.[8] These conditions are further magnified by root causes of inequity[9] such as racism, sexism, heterosexism, and classism. For example, racism is associated with certain types of placements in foster care (for example, youth of color are more likely to be placed in congregate care than their White peers[10]),[11][12], sexism may influence what types of sexual and reproductive health information professionals provide to youth,[13] and heterosexism may result in LGBTQ+ youth not having access to appropriate and relevant sexual health education.[14]
Research finds that sexual and reproductive health outcomes among young people in foster care are worse than among the general population (for example, young people in foster care report first having sex at younger ages than the general population, and young women in foster care experience higher rates of teen pregnancy).[6] However, research also shows that understanding and addressing the ways in which social determinants of health influence the sexual and reproductive health of young people in foster care is imperative to providing them with effective services and improving outcomes related to their sexual and reproductive health. Youth in foster care experience unique conditions that caseworkers and others working within the foster care system should be aware of and mindful toward, such as separation from family of origin, decreased social support,[7] placement instability, and lack of voice and bodily autonomy over medical decisions.[8] These conditions are further magnified by root causes of inequity[9] such as racism, sexism, heterosexism, and classism. For example, racism is associated with certain types of placements in foster care (for example, youth of color are more likely to be placed in congregate care than their White peers[10]),[11][12], sexism may influence what types of sexual and reproductive health information professionals provide to youth,[13] and heterosexism may result in LGBTQ+ youth not having access to appropriate and relevant sexual health education.[14]
In this resource, we define each social determinant of health and describe how it connects to sexual and reproductive health. Then, we discuss how each determinant relates specifically to the sexual and reproductive health and health care experiences of young people involved in foster care; this includes young people in out-of-home care and transitioning out of foster care and into adulthood. Throughout, we provide additional context to highlight inequities within the systems and structures encountered by young people in foster care, many of which may influence their sexual and reproductive health. Last, we provide practice tips for foster care caseworkers to help address barriers related to each social determinant of health. The practice tips for addressing social determinants of health related to sexual and reproductive health are informed by research and by interviews the project team conducted with youth who have lived expertise in foster care and youth-supporting professionals.[a] We also encourage youth-supporting professionals to think about other factors that may influence access to sexual and reproductive health, such as local or state policies (e.g., school district policies on sexual health education) that may introduce further barriers to addressing social determinants of sexual and reproductive health among young people in foster care.
Five Social Determinants of Health
-
1. Neighborhood and built environment
-
2. Education access and quality
-
3. Health care access and quality
-
4. Economic stability
-
5. Social and community context
Practice Tips for Professionals Who Support Youth in Foster Care
This resource has established the parameters for five categories of social determinants of health and described ways in which these determinants impact young people’s sexual and reproductive health—especially for those in foster care. Within this context, we worked with youth-supporting professionals and youth with lived expertise to identify practice tips for navigating social determinants of health when working with youth in foster care. These tips cover various social conditions and inequities that may arise when talking to youth about sexual and reproductive health. Each item features a general practice tip that applies across all social determinants of health, along with an example of how to apply it within specific social determinant categories.
General guidance: Ensure that young people have someone to whom they feel safe speaking about sexual and reproductive health.
Application to health care access and quality and education access and quality: Young people in foster care may not have equitable access to high-quality sexual and reproductive health care education and services.
Caseworkers should help young people identify a medical provider or school staff member with whom they feel safe speaking about sexual and reproductive health, and provide resources to support those conversations. For example, caseworkers can help a young person identify and establish supportive adult relationships in school or establish a relationship with a trusted medical provider. Caseworkers can also provide these trusted adults with information about how to communicate about sexual and reproductive health with young people.
General guidance: Tailor information to individual young people and ensure that these conversations are inclusive of different experiences (e.g., tailored to meet the needs of LGBTQ+ young people).
Application to health care access and quality and social and community context: Young people in foster care are disproportionately youth of color and/or LGBTQ+ youth. They may experience less access to relevant sexual and reproductive health education and services and more discrimination when they receive sexual and reproductive health education and services.
Caseworkers can help young people by providing relevant resources and tailoring sexual and reproductive health information to individual young peoples’ needs, experiences, and communities. For example, caseworkers can provide sexual and reproductive health information to meet the needs of LGBTQ+ young people in ways that are gender-affirming and trauma-responsive.
General guidance: Always make space for youths’ input and let them drive the conversation.
Application to education access and quality: The ways young people in foster care experience and receive education, including sexual and reproductive health education, may influence their belief in their bodily autonomy and the ways in which they experience safety, confidentiality, and consent for care.
Caseworkers can help young people by consistently making space for youths’ input in, and ownership of, conversations about sexual and reproductive health and allowing them to control the conversation. For example, caseworkers can let young people pick the topic of the conversation, ask questions about topics of their choice, and set boundaries on what they do or don’t feel comfortable disclosing.
General guidance: Do not assume anything about the young person’s identity, sexual behaviors, or knowledge.
Application to neighborhood and built environment: Adults often make assumptions about the level of sexual activity, sexual orientation/gender identity, and knowledge about sexual health behaviors among young people in foster care due to biases about the young person’s background.
Caseworkers can help young people by refusing to make assumptions and judgements about young peoples’ identities, sexual behaviors, and knowledge. For example, caseworkers should avoid assumptions about gender and sexual identity, or about whether young people are sexually active, and instead speak with the young person to establish an understanding of their sexual experiences.
General guidance: Ensure that conversations are non-punitive. Young people cannot feel worried that they will get in trouble for being honest.
Application to health care access and quality: Young people in foster care experience challenges in maintaining ownership over their individual decision-making authority and agency due to oppression rooted in inequities across all social determinants of health. Due to this lack of individual autonomy, professionals often find that young people are afraid to be honest about their sexual and reproductive health and health care needs and are concerned about the potentially negative consequences of their honesty.
Caseworkers can help young people by assuring that conversations about sexual and reproductive health are not punitive and remain confidential (unless the topic requires mandated reporting) and ensuring that young people do not experience negative consequences stemming from honest conversations and attempts to seek help. For example, if a young person discloses a risky sexual behavior, caseworkers should ensure that there is not a punishment for that behavior, but rather a discussion of why that behavior could be considered risky and a review of alternative options.
General guidance: Present all available options and let the young person pick what works for them, or what they’re most comfortable with at that moment—even if some options conflict with the caseworker’s personal beliefs.
Application to health care access and quality: Young people in foster care often receive minimal information about sexual and reproductive health due, in part, to limited access to services and education.
Caseworkers can help young people by presenting all available options (e.g., contraceptive options, abortion) and helping them select an appropriately tailored sexual and reproductive health service and/or health aide that makes them feel most comfortable at the time. For example, caseworkers can provide guidance during discussions about the range of contraceptive options, based on youths’ circumstances and interests, or connect the young person with a colleague or medical provider who is able to have such conversations.
General guidance: Ensure that conversations are held in the young person’s preferred language and address language barriers (e.g., offer resources and handouts in the young person’s preferred language, hire an interpreter).
Application to social and community context: Young people in foster care come from racially and ethnically diverse backgrounds and should be given the option to engage in conversations in their preferred language.
Caseworkers can help by ensuring that young people have access to interpreters or linguistically and culturally diverse staff to engage in conversations. For example, if a young person’s preferred language is Spanish, a caseworker should try to find a Spanish-speaking colleague or hire an interpreter if needed. Caseworkers can proactively offer this option to young people and let them decide whether to take advantage.
General guidance: When possible, provide resources to which young people can refer back. Be sure to vet resources provided via social media or other online sources.
Application to health care access and quality: Conversations about sexual and reproductive health can often be overwhelming or sensitive. When young people can access resources for later reference, they face less pressure to remember everything that was discussed.
Caseworkers can help by providing vetted resources to young people on the topics discussed. For example, if a caseworker is discussing birth control options, they may want to provide a resource that summarizes each option.
General guidance: Build a broad network of professionals to connect young people within communities.
Application to social and community context: Young people often have smaller social support networks and experience severed ties to supportive adults due to their system involvement.
Caseworkers can help by cultivating a network of professionals to whom they can connect young people to ensure that youth receive relevant and helpful information. For example, a caseworker might have a pool of approved mentors or other supportive adults with varied lived experiences who have agreed to be connected with young people.
General guidance: Provide preventative care and conversations. Don’t just reach out when something happens.
Application to health care access and quality: Young people in foster care may not have consistent access to preventative health care services such as a yearly pelvic exam.
Caseworkers can help by connecting young people to preventative care while in foster care and ensuring that sexual and reproductive health care is built into case plans and regularly discussed with young people. For example, a caseworker may indicate in a young person’s case plan that they will receive preventative sexual and reproductive health care that is age-appropriate and inclusive while in foster care.
General guidance: Provide access to resources such as transportation or financial support for services.
Application to economic stability: Young people may not have access to reliable transportation or the financial support necessary to access sexual and reproductive health services.
Caseworkers can help by providing transportation to appointments or providing bus passes for young people. Additionally, caseworkers should ensure that young people can afford any copays, prescriptions, or other follow-up needed to access sexual and reproductive health services. For example, a young person may not be able to attend an appointment because they do not have transportation, but a caseworker could drop them off or provide a bus pass.
Suggested citation: Rosenberg, R., Woods, N., Naylon, K., & Tallant, J. (2022). Incorporating social determinants of health and equity in practice to address sexual and reproductive health for young people involved in foster care. Child Trends. https://activatecenter.org/resource/incorporating-social-determinants-of-health-and-equity-in-practice-to-address-sexual-and-reproductive-health-for-young-people-involved-in-foster-care
Footnotes
[a] The project team conducted two interviews with youth with lived expertise and six interviews with youth-supporting professionals (e.g., an independent living specialist, sexual and reproductive health educators, and other direct service practitioners) focused on social determinants of health, sexual and reproductive health care, and how to navigate these factors within the foster care system. All interviews lasted 30 minutes to 1 hour and were conducted virtually via Microsoft Teams.
[b] Cisgender refers to people whose gender identity matches their sex assigned at birth.




